Few years ago when I clocked in my shift at the neonatal ward, I had no idea that I was going to fall in love. For weeks, my rotation felt like heaven working with babies is all that I have always dreamed of. And that day, a tiny human stole my heart. Born prematurely weighing just one kilogram, he was active despite having tubes all over to keep him going.
Even after I left the department, every morning and evening I made sure to pass by and say hi to him. His resilience, courage and persistence was my inspiration. Even on the hard days, when I felt like the world was crumbling down, he kept me going.
There were days I was too exhausted to wake up, the daily journey of Mbezi Temeke drained me physically and mentally, yet the excitement of seeing him took me off the bed to fight for daladala on dark cold mornings just to know that he was okay. After weeks at the neonatal ward, he was discharged on my day off and to be honest he will remain a success story in my heart. That is baby S, the little one who stole my heart.
Baby S is one among many babies that have survived as a result of a well-equipped neonatal intensive care unit (NICU) with fully highly skilled staff. Baby S, was an inspiration for me to take part in the Miles for Mothers marathon prepared by JHPIEGO in collaboration with the Doris Mollel Foundation to fundraise for building and equipping NICU in Kwimba District, Mwanza.
On the 15th of October,2023, I walked 5 kilometers for that cause and when I finally received my medal, I raised it up to dedicate it to the little preemie Baby S who still inspires me today.
RELATED CONTENT:Researchers develop smartphone app to enhance midwifery care in Tanzania
A slow-paced journey
At the end of that marathon, the Director of the Division of Reproductive,Maternal and Child Health, Dr. Ahmad Makuwani mentioned something that stuck with me and picked my interest. “In 2015/16, around 25 babies out of 1,000 live births died. In 2022, this number has only decreased to 24 deaths out of 1,000 live births,” said Makuwani.
I had no idea how little had changed over the years in terms of neonatal mortality. According to the recently released Tanzania Demographic Health Survey (TDHS) 2022 report, the trends of under-5 mortality have decreased significantly, infant mortality has decreased steadily but neonatal mortality has barely changed from 32 deaths per 1,000 live births in 2004-2005 to 24 deaths per 1,000 live births in 2022. Neonatal deaths also account for 73 percent of infant mortality.
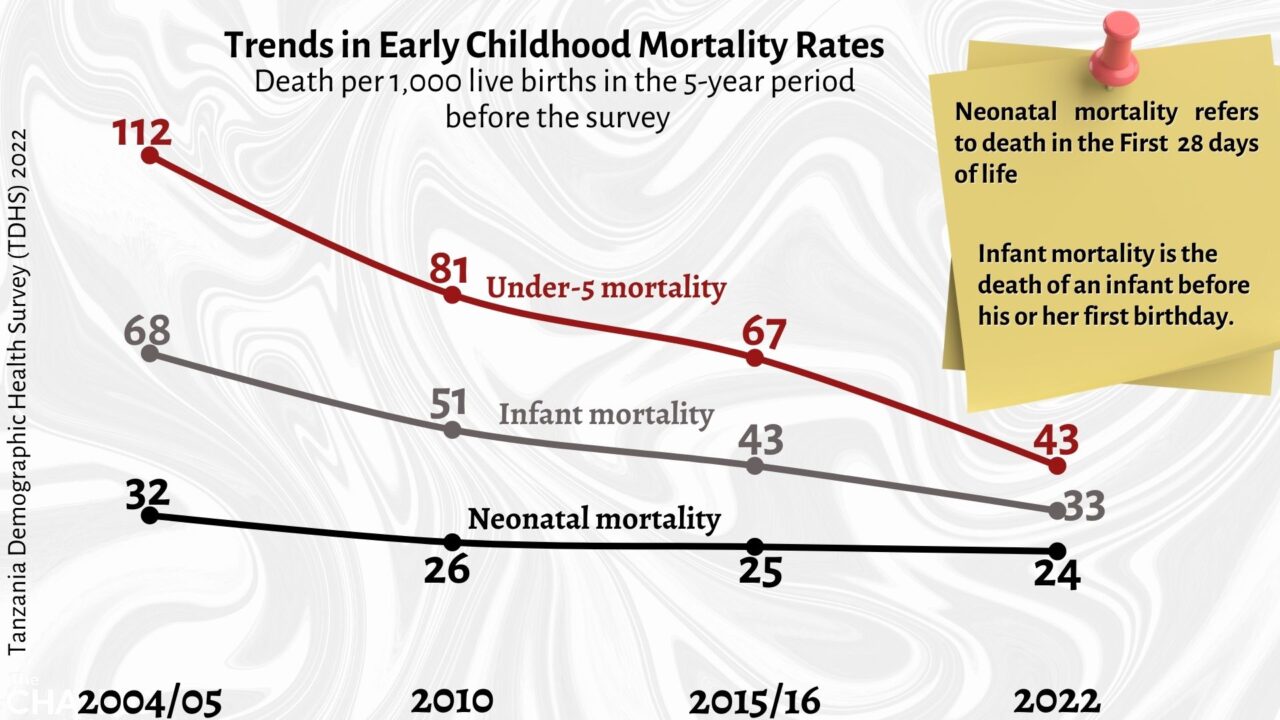
Under-5 mortality rate declined from 112 deaths per 1,000 live births in the 5 years preceding the 2004–05 TDHS to 43 deaths per 1,000 live births in the 5 years preceding the 2022 TDHS-MIS. Over the same period, the infant mortality rate declined from 68 to 33 deaths per 1,000 live births and the neonatal mortality rate declined from 32 to 24 deaths per 1,000 live births. The difference is staggering as the neonatal mortality trends have literally flatlined.
The major causes of neonatal mortality are very much known and that includes, preterm birth, intrapartum-related complications (birth asphyxia or inability to breathe at birth/respiratory distress), infections(sepsis) and birth defects. And the challenges too are very much known, including lack of equipment, inadequate staff and lack of skills.
It worth noting that the issue is starting to attract more attention, like observed during the second Reproductive, Maternal, Newborn, Child and Adolescent Health, and Nutrition (RMNCAH+N) Scientific Conference held at Julius Nyerere Convention Center from 15th to 17th November.One of the presentation that stood out was that from the Vice President of Paediatric Association of Tanzania (PAT), Dr.Theopista Jacob Masenge.
“Our neonatal mortality is 24 deaths per 1,000 live births and in Tanzania an average of 2 million babies are born annually. That means 48,000 neonates die every year, which is 4,000 neonates every month which translates to 143 neonatal deaths per day,” explained Dr Masenge.
“This is equal to three Yutong passengers’ buses with 48 full seats each having an accident and killing everyone per day,” added Dr Masenge.
What is being done to change this?
The Government of Tanzania has recently put efforts to build NICU in many hospitals, this has increased the number of NICU from 18 in 2017 to 175 as of June 2023. Also, 72 health centers and 175 hospitals have specialized Kangaroo Mother Care rooms for children born prematurely and underweight with the goal of reaching a total of 275 health facilities as of June 2024.
Professional associations too have the role in decreasing the neonatal mortality in Tanzania, and this includes the Paediatric Association of Tanzania(PAT) and Tanzania Society of Paediatric Nurses(TSPN). Tanzania has over 400 pediatricians, about 10 neonatologists and 40 pediatric nurses.
PAT works with MOH – RCH to support maternal and perinatal death surveillance and response(MPDSR) activities especially on the perinatal audit. On the other hand, TSPN works with the Ministry of Health and developing partners including USAID Afya Yangu project implemented by JHPIEGO Tanzania by training healthcare providers in newly established NICU on neonatal care.
RELATED CONTENT: Recovering From COVID-19’s Aftermath: Is Tanzania Prepared for Future Infectious Diseases?
Individuals and various organizations such as the Doris Mollel Foundation are taking extra steps to improve the situation. In October 2023, I was part of the panel to discuss review meeting of the locally made Continuous Positive Airway Pressure (CPAP), a machine used to maintain or increase functional residual capacity of the lungs, help prevent alveolar collapse, reduce the work of breathing and improve gas exchange in infants with respiratory distress.
Sandra Sommi, the founder of Plus Life Company is leading the team into producing low cost, high quality biomedical devices including CPAP. When their product is completed, it can be a gamechanger as it is estimated that 20 percent of babies presenting with severe respiratory distress die in low and middle income countries. Even with availability of NICU, medical equipment is inadequate due to high purchasing and maintaining cost.
Beyond the hospital, what can be done?
Tanzania has good policies and strategies regarding neonatal health but the trends of neonatal mortality is proof that this is not good enough to change the neonatal mortality. The Outcome of perinatal mortality is the outcome of maternal care, thus the need for introduction of newborn triage check in maternity wards and close link with maternal and neonatal care.
Training alone is not enough, there is a need for frequent mentorship for capacity building of staff and inclusion of comprehensive newborn care in syllabus. Specialization is important too, hence the need for the government and private institutions to encourage healthcare providers to specialize by provision of scholarships and funding. The NICU team must be separate, and this brings the need for human resources to improve documentation because the goal is not just for the baby to survive, but to thrive hence the need for follow up.
Lest we forget that the Tanzania Employment Act does not specifically recognize the mothers of premature babies separately when it comes to maternity leave. There is a need to change that and provide more than 84 days of maternity leave for mothers with preterm babies.
Last but not least, we need to as Generation Z say “keep the same energy” in neonatal mortality as we do in maternal mortality. Because no way in the same period that maternal mortality dropped by 80% from 530 deaths per 100,000 live births in 2015/16 to 104 deaths per 100,000 live births in 2022; the neonatal mortality dropped by only 4% from 25 deaths per 1000 live births in 2015/16 to 24 deaths per 1000 live births in 2022. What this data says is that we are saving the mothers and forgetting the babies. My message is simple, the child is an extension of the mother, SAVE THEM BOTH.
Kuduishe Kisowile is a medical doctor and public health commentator based in Dar es Salaam, Tanzania. She is available through kuduzekudu@gmail.com or on X as @Kudu_ze_Kudu. Want to publish in this space? Contact our editors at editor@thechanzo.com for further inquiries.




2 responses
Building nicu,without knowledgeable and committed ,government should increase the number of skilled staffs ,and formal training for those staffs especially nurses and doctors, working with neonates.
Building nicu,without knowledgeable and committed ,government should increase the number of skilled staffs ,and formal training for those staffs especially nurses and doctors, working with neonates